Understanding MAFLD (Metabolic Dysfunction–Associated Fatty Liver Disease)
- posted: Sep. 10, 2025
Metabolic dysfunction–associated fatty liver disease (MAFLD) — previously called NAFLD (non-alcoholic fatty liver disease) — is one of the most common liver conditions worldwide. It’s closely linked with modern lifestyle factors such as obesity, diabetes, and metabolic syndrome.
What is MAFLD?
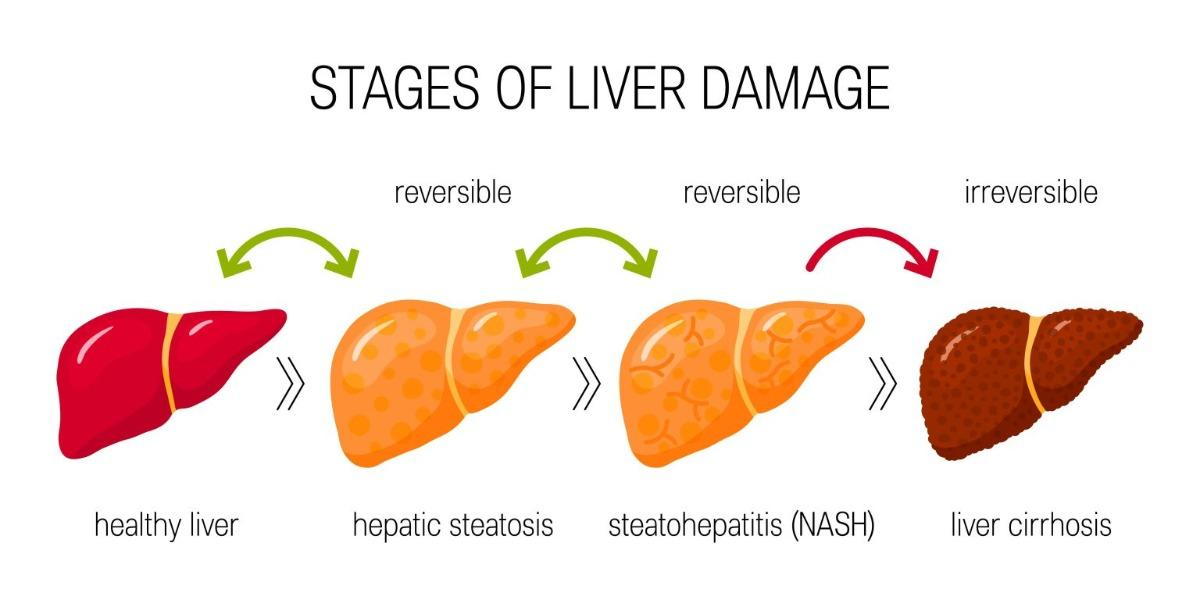
MAFLD happens when extra fat builds up in the liver in people who also have metabolic health problems. Over time, this can lead to liver inflammation, scarring (fibrosis), and in some cases cirrhosis or liver cancer.
Doctors now use the term MAFLD instead of NAFLD because it better reflects the root cause: metabolic dysfunction, rather than just the absence of alcohol use.
How is MAFLD Diagnosed?
Most people with MAFLD don’t have noticeable symptoms. Often, it’s found when routine blood tests show abnormal liver enzymes or when an imaging test (like ultrasound) reveals fatty liver.
Diagnosis usually includes:
Medical history and exam – focusing on weight, diabetes, blood pressure, cholesterol, and alcohol use.
Blood tests – to check liver enzymes and rule out other causes of liver disease.
Imaging – ultrasound, FibroScan (transient elastography), or MRI can measure fat and stiffness in the liver.
Non-invasive scoring systems – such as FIB-4, which estimates the risk of advanced fibrosis.
Liver biopsy (rarely needed) – sometimes performed if there’s uncertainty or suspicion of advanced disease.
Management of MAFLD
The good news is that MAFLD is manageable — and often reversible — with lifestyle changes and medical care.
1. Lifestyle and Diet
Weight loss: Losing 7–10% of body weight can reduce liver fat and inflammation.
Healthy diet: A Mediterranean-style diet (rich in vegetables, fruits, whole grains, lean proteins, and healthy fats) is often recommended.
Limit sugary drinks and processed foods: These contribute to fat buildup in the liver.
2. Exercise
Aim for 150 minutes of moderate activity per week (like brisk walking, swimming, or cycling).
Both aerobic and resistance training can improve liver health.
3. Managing Metabolic Risks
Diabetes control – keeping blood sugar in target range.
Cholesterol management – statins are safe for most people with MAFLD.
Blood pressure control.
Weight loss
4. Medications and New Therapies
Currently, no specific drug is FDA-approved for MAFLD.
Some patients may benefit from medications that target diabetes (like GLP-1 receptor agonists or pioglitazone).
Clinical trials are ongoing for new liver-specific treatments.
5. Regular Monitoring
People with MAFLD should be followed by their primary care provider or gastroenterologist/hepatologist.
Monitoring includes repeat labs, imaging, and sometimes FibroScan to check for progression.
MAFLD is common, but with early diagnosis and consistent lifestyle changes, most people can stop progression — and even reverse damage. If you’ve been told you have fatty liver, don’t panic: work with your healthcare provider to make sustainable changes and monitor your liver health.

- posted: Sep. 10, 2025
Metabolic dysfunction–associated fatty liver disease (MAFLD) — previously called NAFLD (non-alcoholic fatty liver disease) — is one of the most common liver conditions worldwide. It’s closely linked with modern lifestyle factors such as obesity, diabetes, and metabolic syndrome.
What is MAFLD?
MAFLD happens when extra fat builds up in the liver in people who also have metabolic health problems. Over time, this can lead to liver inflammation, scarring (fibrosis), and in some cases cirrhosis or liver cancer.
Doctors now use the term MAFLD instead of NAFLD because it better reflects the root cause: metabolic dysfunction, rather than just the absence of alcohol use.
How is MAFLD Diagnosed?
Most people with MAFLD don’t have noticeable symptoms. Often, it’s found when routine blood tests show abnormal liver enzymes or when an imaging test (like ultrasound) reveals fatty liver.
Diagnosis usually includes:
Medical history and exam – focusing on weight, diabetes, blood pressure, cholesterol, and alcohol use.
Blood tests – to check liver enzymes and rule out other causes of liver disease.
Imaging – ultrasound, FibroScan (transient elastography), or MRI can measure fat and stiffness in the liver.
Non-invasive scoring systems – such as FIB-4, which estimates the risk of advanced fibrosis.
Liver biopsy (rarely needed) – sometimes performed if there’s uncertainty or suspicion of advanced disease.
Management of MAFLD
The good news is that MAFLD is manageable — and often reversible — with lifestyle changes and medical care.
1. Lifestyle and Diet
Weight loss: Losing 7–10% of body weight can reduce liver fat and inflammation.
Healthy diet: A Mediterranean-style diet (rich in vegetables, fruits, whole grains, lean proteins, and healthy fats) is often recommended.
Limit sugary drinks and processed foods: These contribute to fat buildup in the liver.
2. Exercise
Aim for 150 minutes of moderate activity per week (like brisk walking, swimming, or cycling).
Both aerobic and resistance training can improve liver health.
3. Managing Metabolic Risks
Diabetes control – keeping blood sugar in target range.
Cholesterol management – statins are safe for most people with MAFLD.
Blood pressure control.
Weight loss
4. Medications and New Therapies
Currently, no specific drug is FDA-approved for MAFLD.
Some patients may benefit from medications that target diabetes (like GLP-1 receptor agonists or pioglitazone).
Clinical trials are ongoing for new liver-specific treatments.
5. Regular Monitoring
People with MAFLD should be followed by their primary care provider or gastroenterologist/hepatologist.
Monitoring includes repeat labs, imaging, and sometimes FibroScan to check for progression.
MAFLD is common, but with early diagnosis and consistent lifestyle changes, most people can stop progression — and even reverse damage. If you’ve been told you have fatty liver, don’t panic: work with your healthcare provider to make sustainable changes and monitor your liver health.
