Alcohol-Related Liver Disease (ALD): Symptoms, Diagnosis, and Treatment
- posted: Dec. 02, 2025
Alcohol-related liver disease (ALD) is one of the most common causes of chronic liver disease worldwide. It occurs when long-term or heavy alcohol use damages the liver, leading to inflammation, scarring, and impaired function. If not addressed early, ALD can progress to cirrhosis or even liver failure.
What is Alcohol-Related Liver Disease?
Alcohol-related liver disease refers to liver damage caused specifically by excessive or prolonged alcohol consumption. The liver is responsible for breaking down alcohol, but over time, toxic byproducts can create inflammation and injury to liver cells.
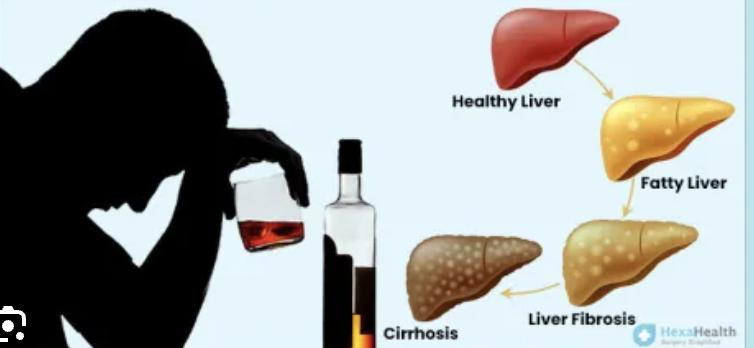
There are three main stages of ALD, which can exist separately or overlap:
- Alcoholic Fatty Liver Disease (Steatosis) – early accumulation of fat in the liver
- Alcoholic Hepatitis – inflammation and liver cell damage
- Alcohol-Related Cirrhosis – advanced scarring that permanently impairs liver function
Genetics, nutrition, amount/duration of alcohol intake, and coexisting conditions (like obesity or viral hepatitis) all influence risk.
Symptoms of Alcohol-Related Liver Disease
Symptoms vary depending on the stage of the disease. Many people with early ALD have no symptoms.
Common symptoms include:
Early-Stage ALD (Fatty Liver)
- Fatigue
- Decreased appetite
- Mild discomfort in the right upper abdomen
Alcoholic Hepatitis
- Jaundice (yellowing of the skin/eyes)
- Abdominal pain or tenderness
- Fever
- Nausea or vomiting
- Loss of appetite
- Rapid weight loss or muscle wasting
Alcohol-Related Cirrhosis
- Abdominal swelling (ascites)
- Confusion or brain fog (hepatic encephalopathy)
- Easy bruising or bleeding
- Severe fatigue
- Swelling in the legs
- Dark urine or pale stools
If you or someone you know experiences signs of severe alcoholic hepatitis—such as jaundice, abdominal pain, or vomiting—seek medical care immediately.
How is Alcohol-Related Liver Disease Diagnosed?
There is no single test for ALD. Diagnosis is based on history, laboratory results, imaging, and ruling out other causes of liver disease.
Common Diagnostic Steps
- Medical history and physical exam – including alcohol intake patterns and risk factors
- Blood tests – liver enzymes, bilirubin, platelet count, INR, and markers of inflammation
- Ultrasound – to evaluate liver texture, size, and presence of steatosis or cirrhosis
- FibroScan (elastography) – measures liver stiffness to assess fibrosis or scarring
- CT or MRI – if more detailed imaging is needed
- Liver biopsy – rarely needed but can confirm inflammation or fibrosis when diagnosis is uncertain
Your provider may also test for viral hepatitis, autoimmune markers, metabolic disorders, or iron overload to rule out other liver conditions.
Managing Alcohol-Related Liver Disease
The most important step in treating ALD is complete abstinence from alcohol, which can stop progression and even reverse early liver damage. Additional medical treatments and lifestyle changes support recovery.
1. Alcohol Cessation
Stopping alcohol use is the cornerstone of treatment. Options include:
- Counseling or therapy
- Medication-assisted treatment (e.g., naltrexone, acamprosate, disulfiram)
- Support groups (AA, SMART Recovery)
- Inpatient or outpatient detox programs for withdrawal management
Early cessation significantly improves survival and long-term liver health.
2. Nutritional Support
Malnutrition is common in ALD.
Recommended strategies:
- High-protein diet to maintain muscle mass
- Vitamin supplementation (especially thiamine, folate, and B-complex)
- Avoiding fasting or skipping meals
- Working with a dietitian to customize meal planning
3. Medications
Depending on disease severity, your provider may recommend:
- Steroids – sometimes used for severe alcoholic hepatitis
- Diuretics – to manage fluid buildup (ascites)
- Lactulose or rifaximin – for encephalopathy
- Antioxidants or anti-inflammatory therapies – in select cases
These are tailored to each individual's condition and response.
4. Management of Complications
If cirrhosis is present, ongoing monitoring is essential:
- Ultrasound every 6 months for liver cancer screening (HCC)
- Endoscopy for variceal screening
- Routine labs to track liver function and progression
- Sodium restriction for ascites
- Avoiding NSAIDs, which increase bleeding risk
5. Liver Transplant Evaluation
For advanced cirrhosis or severe alcoholic hepatitis not responding to treatment, a liver transplant evaluation may be considered. Many transplant centers require documented sobriety and participation in a recovery program.
Living with Alcohol-Related Liver Disease
With early diagnosis and complete alcohol cessation, many people with ALD can stabilize their liver function—and in some cases reverse early damage. Regular follow-up with your healthcare provider, supportive lifestyle changes, and ongoing monitoring are key to long-term health.
If you’re experiencing symptoms or concerned about alcohol’s impact on your liver, don’t wait. Early evaluation and treatment can be life-saving and help protect your liver for the future.

- posted: Dec. 02, 2025
Alcohol-related liver disease (ALD) is one of the most common causes of chronic liver disease worldwide. It occurs when long-term or heavy alcohol use damages the liver, leading to inflammation, scarring, and impaired function. If not addressed early, ALD can progress to cirrhosis or even liver failure.
What is Alcohol-Related Liver Disease?
Alcohol-related liver disease refers to liver damage caused specifically by excessive or prolonged alcohol consumption. The liver is responsible for breaking down alcohol, but over time, toxic byproducts can create inflammation and injury to liver cells.
There are three main stages of ALD, which can exist separately or overlap:
- Alcoholic Fatty Liver Disease (Steatosis) – early accumulation of fat in the liver
- Alcoholic Hepatitis – inflammation and liver cell damage
- Alcohol-Related Cirrhosis – advanced scarring that permanently impairs liver function
Genetics, nutrition, amount/duration of alcohol intake, and coexisting conditions (like obesity or viral hepatitis) all influence risk.
Symptoms of Alcohol-Related Liver Disease
Symptoms vary depending on the stage of the disease. Many people with early ALD have no symptoms.
Common symptoms include:
Early-Stage ALD (Fatty Liver)
- Fatigue
- Decreased appetite
- Mild discomfort in the right upper abdomen
Alcoholic Hepatitis
- Jaundice (yellowing of the skin/eyes)
- Abdominal pain or tenderness
- Fever
- Nausea or vomiting
- Loss of appetite
- Rapid weight loss or muscle wasting
Alcohol-Related Cirrhosis
- Abdominal swelling (ascites)
- Confusion or brain fog (hepatic encephalopathy)
- Easy bruising or bleeding
- Severe fatigue
- Swelling in the legs
- Dark urine or pale stools
If you or someone you know experiences signs of severe alcoholic hepatitis—such as jaundice, abdominal pain, or vomiting—seek medical care immediately.
How is Alcohol-Related Liver Disease Diagnosed?
There is no single test for ALD. Diagnosis is based on history, laboratory results, imaging, and ruling out other causes of liver disease.
Common Diagnostic Steps
- Medical history and physical exam – including alcohol intake patterns and risk factors
- Blood tests – liver enzymes, bilirubin, platelet count, INR, and markers of inflammation
- Ultrasound – to evaluate liver texture, size, and presence of steatosis or cirrhosis
- FibroScan (elastography) – measures liver stiffness to assess fibrosis or scarring
- CT or MRI – if more detailed imaging is needed
- Liver biopsy – rarely needed but can confirm inflammation or fibrosis when diagnosis is uncertain
Your provider may also test for viral hepatitis, autoimmune markers, metabolic disorders, or iron overload to rule out other liver conditions.
Managing Alcohol-Related Liver Disease
The most important step in treating ALD is complete abstinence from alcohol, which can stop progression and even reverse early liver damage. Additional medical treatments and lifestyle changes support recovery.
1. Alcohol Cessation
Stopping alcohol use is the cornerstone of treatment. Options include:
- Counseling or therapy
- Medication-assisted treatment (e.g., naltrexone, acamprosate, disulfiram)
- Support groups (AA, SMART Recovery)
- Inpatient or outpatient detox programs for withdrawal management
Early cessation significantly improves survival and long-term liver health.
2. Nutritional Support
Malnutrition is common in ALD.
Recommended strategies:
- High-protein diet to maintain muscle mass
- Vitamin supplementation (especially thiamine, folate, and B-complex)
- Avoiding fasting or skipping meals
- Working with a dietitian to customize meal planning
3. Medications
Depending on disease severity, your provider may recommend:
- Steroids – sometimes used for severe alcoholic hepatitis
- Diuretics – to manage fluid buildup (ascites)
- Lactulose or rifaximin – for encephalopathy
- Antioxidants or anti-inflammatory therapies – in select cases
These are tailored to each individual's condition and response.
4. Management of Complications
If cirrhosis is present, ongoing monitoring is essential:
- Ultrasound every 6 months for liver cancer screening (HCC)
- Endoscopy for variceal screening
- Routine labs to track liver function and progression
- Sodium restriction for ascites
- Avoiding NSAIDs, which increase bleeding risk
5. Liver Transplant Evaluation
For advanced cirrhosis or severe alcoholic hepatitis not responding to treatment, a liver transplant evaluation may be considered. Many transplant centers require documented sobriety and participation in a recovery program.
Living with Alcohol-Related Liver Disease
With early diagnosis and complete alcohol cessation, many people with ALD can stabilize their liver function—and in some cases reverse early damage. Regular follow-up with your healthcare provider, supportive lifestyle changes, and ongoing monitoring are key to long-term health.
If you’re experiencing symptoms or concerned about alcohol’s impact on your liver, don’t wait. Early evaluation and treatment can be life-saving and help protect your liver for the future.
