Hiatal Hernia: Symptoms, Causes, Diagnosis, and Treatment
- posted: Dec. 10, 2025
A hiatal hernia is a common condition in which part of the stomach pushes up into the chest through an opening in the diaphragm. While many people never develop symptoms, others experience significant reflux, discomfort, and impaired quality of life. Early evaluation and targeted treatment can prevent progression and reduce complications.
What Is a Hiatal Hernia?
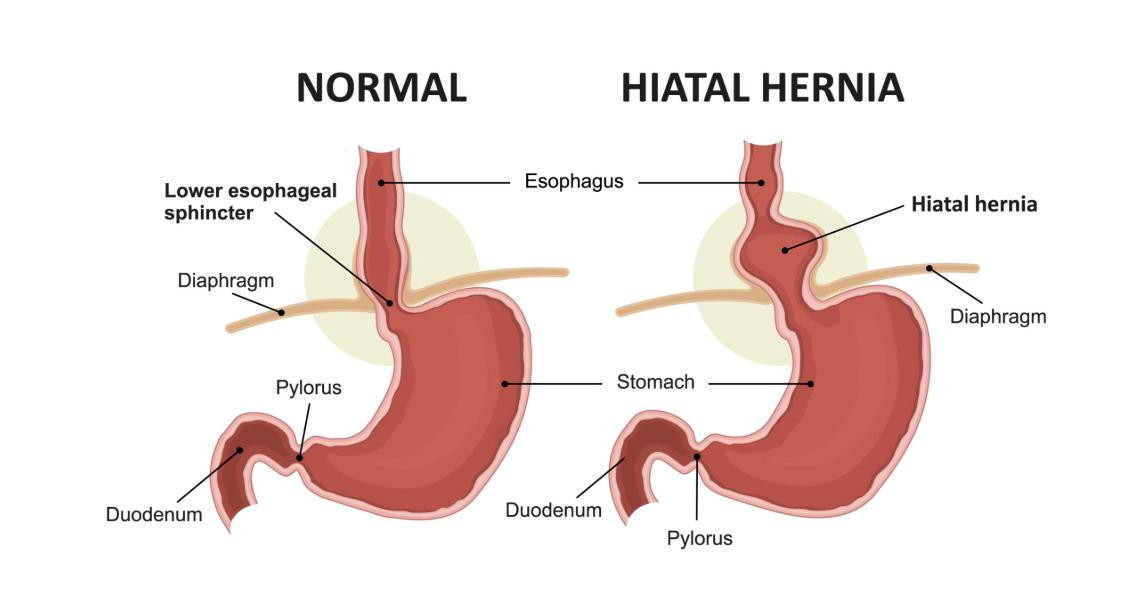
A hiatal hernia occurs when the upper part of the stomach moves through the diaphragmatic hiatus and into the chest cavity. The diaphragm normally helps keep stomach acid contained, but when the hiatus becomes weakened or enlarged, the stomach can slide upward and contribute to reflux.
There are two main types of hiatal hernias:
Sliding Hiatal Hernia – The most common type. The stomach and lower esophageal sphincter (LES) move into the chest, increasing the likelihood of acid reflux and GERD.
Paraesophageal (Rolling) Hernia – Less common but more serious. Part of the stomach herniates alongside the esophagus and can become trapped or twisted.
Risk factors include age-related muscle weakening, obesity, chronic coughing, smoking, pregnancy, and repetitive straining.
Symptoms of a Hiatal Hernia
Symptoms depend on the type and size of the hernia. Some individuals have no symptoms, particularly with small sliding hernias.
Common symptoms include:
Mild or Early Symptoms
- Heartburn or acid reflux
- Regurgitation of food or acid
- Burping or bloating
- Mild chest or upper abdominal discomfort
Moderate Symptoms
- Difficulty swallowing (dysphagia)
- A sensation of food “sticking”
Severe or Paraesophageal Hernia Symptoms
- Significant chest pain or pressure
- Shortness of breath
- Early fullness when eating
- Vomiting or inability to tolerate food
- Gastrointestinal bleeding (rare)
How Is a Hiatal Hernia Diagnosed?
There is no single test that diagnoses all hiatal hernias. Providers use a combination of clinical assessment and imaging to confirm the condition.
Common Diagnostic Steps
Medical history and physical exam – evaluating reflux symptoms, swallowing issues, or risk factors.
- Upper endoscopy (EGD) – visualizes the esophagus, stomach, and presence of a hernia.
- Barium swallow (upper GI series) – outlines anatomy and shows the hernia’s size and position
- Esophageal manometry – measures esophageal function and LES pressure.
- pH testing – assesses acid exposure in patients with suspected GERD.
- CT scan – may incidentally identify a hiatal hernia.
These evaluations help determine the type of hernia and guide treatment.
Managing a Hiatal Hernia
Treatment depends on the severity of symptoms and the type of hernia. Many patients improve with lifestyle modifications and acid-suppressing therapy, while others may require surgical repair.
1. Lifestyle Modifications
These strategies reduce reflux and symptom severity:
- Eat smaller, more frequent meals
- Avoid lying down within 2–3 hours after eating
- Elevate the head of the bed
- Limit caffeine, alcohol, spicy foods, and acidic foods
- Avoid tight clothing around the abdomen
- Achieve and maintain a healthy weight
- Stop smoking
Lifestyle measures are essential even when using medication.
2. Medications
Medications focus on controlling reflux and reducing stomach acid:
- Proton pump inhibitors (PPIs)
- H₂ blockers
- Antacids
- Prokinetic agents (in select cases)
These help reduce irritation and prevent complications such as esophagitis.
3. Management of Complications
Patients with significant reflux or advanced symptoms may require:
- Routine endoscopy for chronic GERD or Barrett’s esophagus
- Dietary adjustments to treat dysphagia
- Treatment of anemia if gastrointestinal bleeding is present
- Monitoring for aspiration-related respiratory symptoms
4. Surgical Intervention
Surgery is considered when:
- Symptoms persist despite maximal medical therapy
- The hernia is large or paraesophageal
- Complications such as bleeding, volvulus, or obstruction occur
Laparoscopic hiatal hernia repair with fundoplication is the most common surgical approach. It reinforces the LES and restores the stomach to the abdominal cavity.
Living with a Hiatal Hernia
Many patients can successfully manage hiatal hernia symptoms through targeted lifestyle modifications and acid-suppressing therapy. With appropriate care, long-term complications—such as esophagitis, Barrett’s esophagus, chronic GERD, and swallowing difficulties—can often be reduced or prevented. Ongoing follow-up with a Gastroenterologist allows for careful monitoring, timely diagnostic evaluation, and personalized treatment strategies tailored to each patient’s needs.
If you are experiencing reflux, difficulty swallowing, persistent upper abdominal discomfort, or symptoms not improving with over-the-counter medication, our team at Gastrointestinal and Liver Consultants can provide a comprehensive assessment. Early evaluation helps confirm the presence of a hiatal hernia and ensures you receive the most effective, evidence-based treatment options.

- posted: Dec. 10, 2025
A hiatal hernia is a common condition in which part of the stomach pushes up into the chest through an opening in the diaphragm. While many people never develop symptoms, others experience significant reflux, discomfort, and impaired quality of life. Early evaluation and targeted treatment can prevent progression and reduce complications.
What Is a Hiatal Hernia?
A hiatal hernia occurs when the upper part of the stomach moves through the diaphragmatic hiatus and into the chest cavity. The diaphragm normally helps keep stomach acid contained, but when the hiatus becomes weakened or enlarged, the stomach can slide upward and contribute to reflux.
There are two main types of hiatal hernias:
Sliding Hiatal Hernia – The most common type. The stomach and lower esophageal sphincter (LES) move into the chest, increasing the likelihood of acid reflux and GERD.
Paraesophageal (Rolling) Hernia – Less common but more serious. Part of the stomach herniates alongside the esophagus and can become trapped or twisted.
Risk factors include age-related muscle weakening, obesity, chronic coughing, smoking, pregnancy, and repetitive straining.
Symptoms of a Hiatal Hernia
Symptoms depend on the type and size of the hernia. Some individuals have no symptoms, particularly with small sliding hernias.
Common symptoms include:
Mild or Early Symptoms
- Heartburn or acid reflux
- Regurgitation of food or acid
- Burping or bloating
- Mild chest or upper abdominal discomfort
Moderate Symptoms
- Difficulty swallowing (dysphagia)
- A sensation of food “sticking”
Severe or Paraesophageal Hernia Symptoms
- Significant chest pain or pressure
- Shortness of breath
- Early fullness when eating
- Vomiting or inability to tolerate food
- Gastrointestinal bleeding (rare)
How Is a Hiatal Hernia Diagnosed?
There is no single test that diagnoses all hiatal hernias. Providers use a combination of clinical assessment and imaging to confirm the condition.
Common Diagnostic Steps
Medical history and physical exam – evaluating reflux symptoms, swallowing issues, or risk factors.
- Upper endoscopy (EGD) – visualizes the esophagus, stomach, and presence of a hernia.
- Barium swallow (upper GI series) – outlines anatomy and shows the hernia’s size and position
- Esophageal manometry – measures esophageal function and LES pressure.
- pH testing – assesses acid exposure in patients with suspected GERD.
- CT scan – may incidentally identify a hiatal hernia.
These evaluations help determine the type of hernia and guide treatment.
Managing a Hiatal Hernia
Treatment depends on the severity of symptoms and the type of hernia. Many patients improve with lifestyle modifications and acid-suppressing therapy, while others may require surgical repair.
1. Lifestyle Modifications
These strategies reduce reflux and symptom severity:
- Eat smaller, more frequent meals
- Avoid lying down within 2–3 hours after eating
- Elevate the head of the bed
- Limit caffeine, alcohol, spicy foods, and acidic foods
- Avoid tight clothing around the abdomen
- Achieve and maintain a healthy weight
- Stop smoking
Lifestyle measures are essential even when using medication.
2. Medications
Medications focus on controlling reflux and reducing stomach acid:
- Proton pump inhibitors (PPIs)
- H₂ blockers
- Antacids
- Prokinetic agents (in select cases)
These help reduce irritation and prevent complications such as esophagitis.
3. Management of Complications
Patients with significant reflux or advanced symptoms may require:
- Routine endoscopy for chronic GERD or Barrett’s esophagus
- Dietary adjustments to treat dysphagia
- Treatment of anemia if gastrointestinal bleeding is present
- Monitoring for aspiration-related respiratory symptoms
4. Surgical Intervention
Surgery is considered when:
- Symptoms persist despite maximal medical therapy
- The hernia is large or paraesophageal
- Complications such as bleeding, volvulus, or obstruction occur
Laparoscopic hiatal hernia repair with fundoplication is the most common surgical approach. It reinforces the LES and restores the stomach to the abdominal cavity.
Living with a Hiatal Hernia
Many patients can successfully manage hiatal hernia symptoms through targeted lifestyle modifications and acid-suppressing therapy. With appropriate care, long-term complications—such as esophagitis, Barrett’s esophagus, chronic GERD, and swallowing difficulties—can often be reduced or prevented. Ongoing follow-up with a Gastroenterologist allows for careful monitoring, timely diagnostic evaluation, and personalized treatment strategies tailored to each patient’s needs.
If you are experiencing reflux, difficulty swallowing, persistent upper abdominal discomfort, or symptoms not improving with over-the-counter medication, our team at Gastrointestinal and Liver Consultants can provide a comprehensive assessment. Early evaluation helps confirm the presence of a hiatal hernia and ensures you receive the most effective, evidence-based treatment options.
